Healthcare organizations now operate within highly digitized environments where clinical care, diagnostics, pharmacy services, and financial operations are coordinated through shared information systems. In such environments, operational continuity is closely tied to the stability of the digital platforms through which these workflows interact.
The Hospital Management System increasingly functions as the transactional layer connecting these activities. Clinical documentation, diagnostic orders, medication records, admission processes, and billing transactions are captured and exchanged through the same system environment.
Because these workflows depend on synchronized access to shared data, system availability directly influences the hospital’s ability to maintain clinical workflow continuity and coordinated operational oversight.
Infrastructure instability—whether related to network failures, cybersecurity incidents, hardware outages, or infrastructure maintenance events—therefore introduces operational risk beyond the technology layer.
In digitally integrated hospitals, infrastructure resilience becomes inseparable from operational resilience.
For hospital leadership teams evaluating technology platforms, this reality has elevated the role of system architecture, infrastructure design, and disaster recovery strategy in technology decision-making.
Cloud-native Hospital Management Systems, supported by structured disaster recovery frameworks, offer healthcare organizations a way to strengthen the resilience of their digital health infrastructure while sustaining operational continuity when unexpected events occur.
Understanding the Operational Risks Facing Hospital Technology Environments
Hospital technology ecosystems operate within complex infrastructure environments that include networks, databases, application platforms, diagnostic systems, and external integration layers.
While these environments are designed for reliability, they remain exposed to a range of operational risks.
Use Cases include:
- Network connectivity disruptions affecting application access
- Infrastructure failures within server or storage environments
- Data center outages or power disruptions
- Cybersecurity incidents targeting healthcare systems
- Performance degradation during periods of peak operational demand
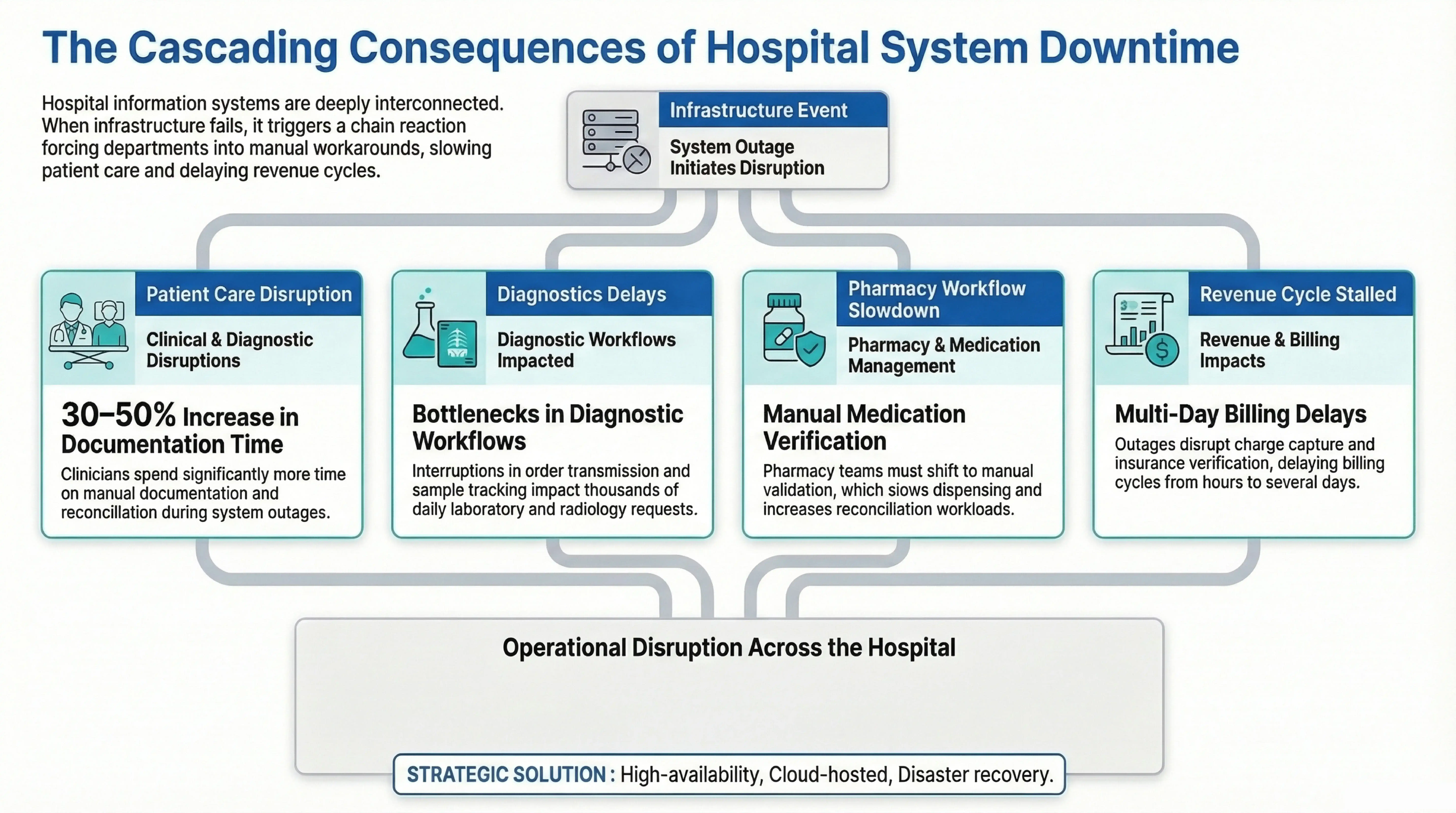
Because hospital systems interact across multiple operational domains, disruptions rarely remain isolated to a single application.
Clinical services, diagnostic departments, pharmacy systems, and revenue cycle platforms often depend on the same infrastructure layers. As a result, infrastructure instability can propagate across the broader system environment.
The operational challenge is therefore not only preventing disruptions—but ensuring that systems are designed to sustain operations when disruptions occur.
Limitations of Traditional On-Premise Healthcare Infrastructure
Many hospital systems were historically deployed within on-premise infrastructure environments, where applications and databases operated on servers located within the hospital facility or within a dedicated local data center.
This model offered control over hardware environments but also introduced structural limitations.
Single-site infrastructure creates a concentration of operational risk, where system availability depends on the stability of a single computing environment.
Common constraints include:
- Dependence on a single data center location
- Limited infrastructure redundancy in smaller IT environments
- Extended recovery timelines following hardware failure
- Capacity limitations during periods of increased system usage
As healthcare organizations expanded their digital capabilities—integrating imaging platforms, diagnostic systems, and patient engagement applications—these constraints became more visible.
Infrastructure resilience therefore began to emerge as a strategic consideration rather than simply an IT operational concern.
The Role of Cloud-Native Hospital Management Systems
Cloud-native architecture introduces a different system design model in which hospital applications are built specifically to operate within distributed cloud environments rather than being adapted from traditional server-based systems.
Under this approach, the HMS platform is architected as a collection of scalable services operating across resilient cloud infrastructure environments.
These environments typically provide:
- Distributed computing infrastructure across multiple availability zones
- Automated resource scaling based on operational demand
- Containerized application environments that support flexible deployment
- Continuous infrastructure monitoring and automated management
Because cloud-native systems are designed for distributed environments from the beginning, they are inherently better suited to support resilience, scalability, and operational continuity.
By operating within such environments, hospitals reduce the operational risks associated with maintaining infrastructure within a single location.
Cloud-native environments also allow infrastructure operations—such as resource allocation, system monitoring, patch management, and performance optimization—to be handled through automated cloud services.
This allows hospital IT teams to focus more directly on clinical system performance, integration management, and operational workflows.
Designing High Availability in Cloud-Native Healthcare Platforms
Beyond infrastructure hosting, system architecture plays an important role in determining how effectively hospital systems remain available during infrastructure events.
Cloud-native architectures are typically designed with high availability as a foundational principle.
High availability architecture focuses on ensuring that application services remain accessible even when individual components of the infrastructure encounter disruption.
Key design approaches may include:
- Distributed application services operating across multiple cloud environments
- Database replication across geographically separated infrastructure zones
- Load balancing to distribute system traffic across service clusters
- Continuous monitoring of infrastructure and application performance
These architectural mechanisms reduce the likelihood that infrastructure events will immediately translate into system outages.
High availability design shifts the focus from single-system reliability to distributed infrastructure resilience.
For hospital operations that depend on continuous system access, this approach allows clinical and operational workflows to continue functioning even during infrastructure instability.
Strengthening Patient Data Resilience Through Disaster Recovery
While high availability architecture focuses on maintaining system accessibility, disaster recovery strategies address scenarios where systems must be restored following major disruptions.
In healthcare environments, disaster recovery planning focuses on protecting both clinical data and operational records.
Core disaster recovery mechanisms may include:
- Automated database backup systems
- Replication of clinical data across distributed infrastructure environments
- Defined recovery time objectives (RTO) for system restoration
- Recovery point objectives (RPO) that limit potential data loss
These mechanisms strengthen patient data resilience, ensuring that critical clinical documentation, diagnostic reports, medication records, and financial transactions remain recoverable even following infrastructure failures.
Protecting Clinical Workflow Continuity
System availability ultimately matters because hospital workflows depend on continuous access to information.
Clinical teams rely on digital platforms to:
- Access patient histories and diagnostic results
- Document consultations and treatment decisions
- Manage medication orders and pharmacy records
- Coordinate care across departments
Operational teams similarly depend on system visibility to coordinate admissions, discharges, bed allocation, and service utilization.
Maintaining system availability therefore directly supports clinical workflow continuity, enabling hospital teams to operate within coordinated information environments.
What Hospital Leaders Should Evaluate in Healthcare Technology Platforms
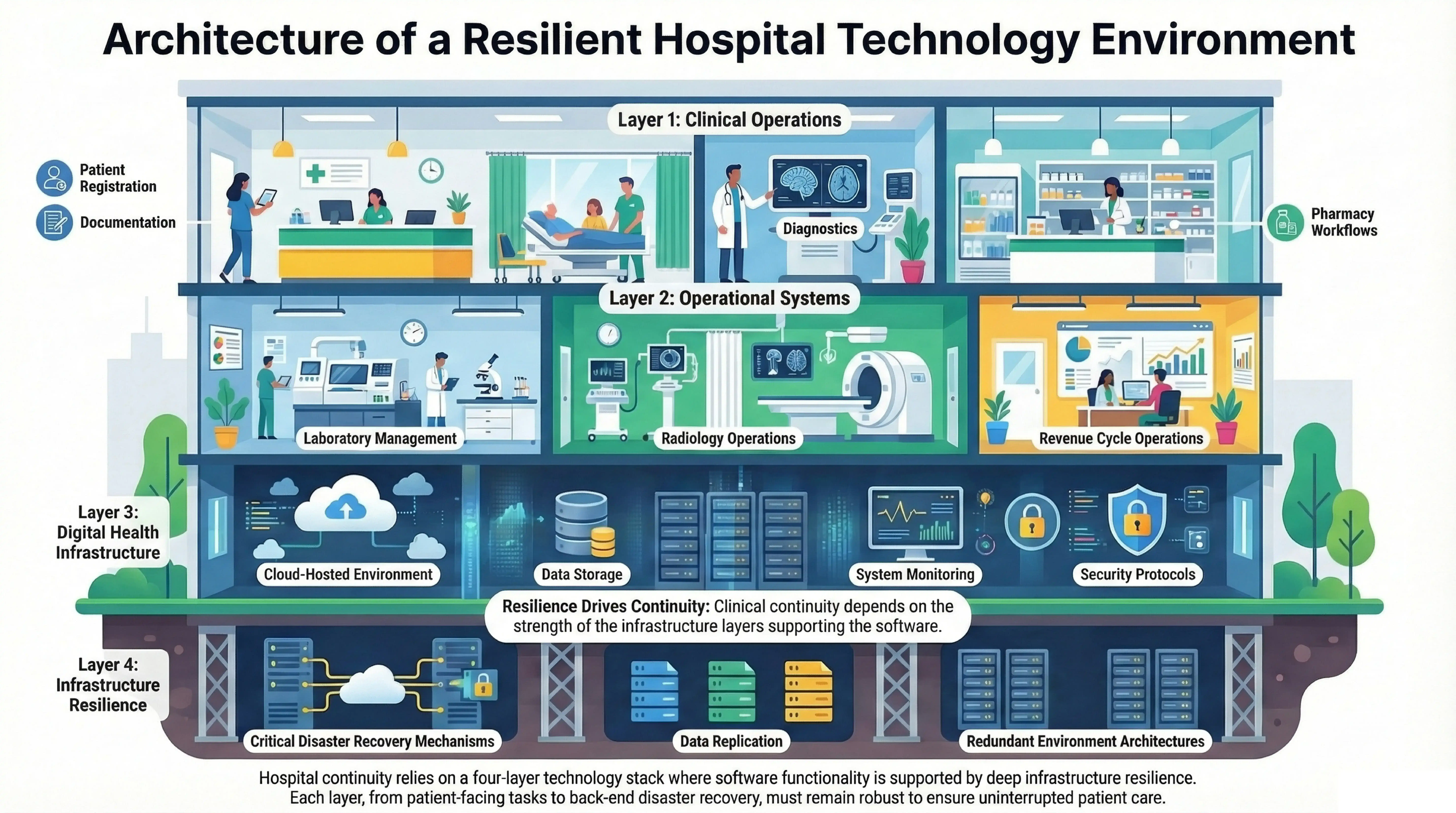
As digital systems become central to hospital operations, leadership teams increasingly evaluate technology platforms through the lens of infrastructure resilience.
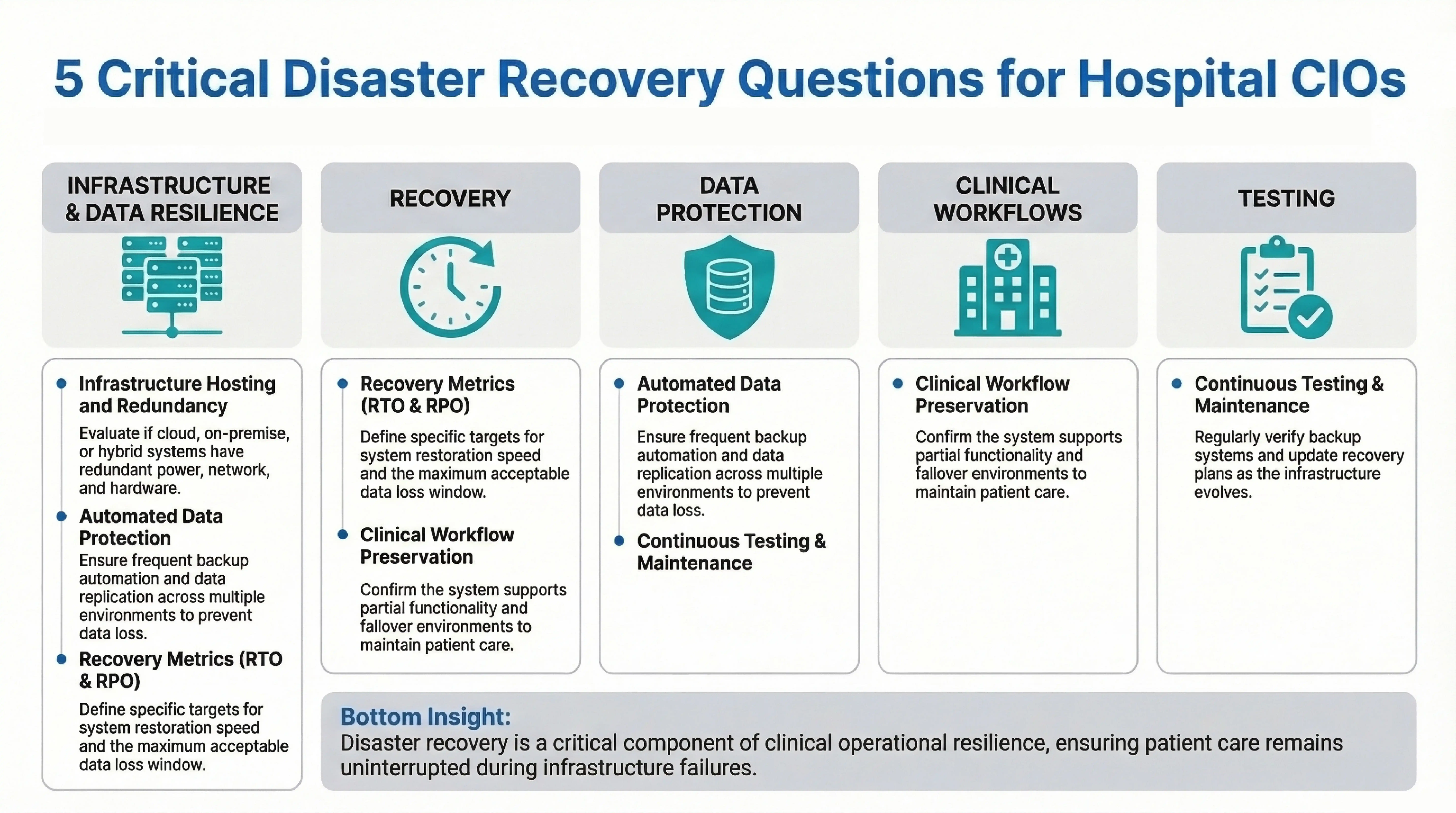
Important considerations may include:
- Is the platform built on cloud-native architecture designed for distributed environments?
- What redundancy mechanisms protect system availability?
- How is clinical and operational data protected against loss?
- What disaster recovery procedures support system restoration?
- How quickly can systems recover following infrastructure disruption?
These questions help determine whether a platform can function as a high-availability healthcare platform capable of sustaining operations in complex digital environments.
Building Resilient Digital Health Infrastructure for the Future
Healthcare delivery continues to evolve toward increasingly digitized clinical environments where information systems coordinate the majority of operational workflows.
Hospital Management Systems now support:
- clinical documentation
- diagnostic and imaging workflows
- pharmacy operations
- revenue cycle management
- operational reporting and oversight
The resilience of the infrastructure supporting these systems therefore plays a central role in sustaining hospital operations.
Technology architecture is increasingly becoming part of the hospital’s operational risk strategy.
Cloud-native Hospital Management Systems, combined with structured disaster recovery frameworks, provide healthcare organizations with a practical pathway toward strengthening their digital health infrastructure.
By operating within distributed cloud environments and implementing structured recovery strategies, hospitals can improve their ability to maintain system availability, protect patient information, and sustain operational continuity when unexpected events occur.
Infrastructure Architecture as a Strategic Decision for Hospital Leadership
Historically, decisions about hospital IT infrastructure were often treated as technical procurement discussions handled primarily within the IT department. As digital systems have become central to clinical and operational workflows, however, the architectural design of those systems increasingly carries organizational implications that extend beyond technology teams.
Hospital Management Systems now coordinate activities that influence patient throughput, clinical documentation, diagnostic workflows, pharmacy operations, and revenue cycle performance.
Because these activities are interconnected through shared digital platforms, infrastructure decisions directly influence the hospital’s ability to maintain stable operations.
For this reason, infrastructure architecture is gradually becoming part of executive-level operational planning.
Hospital leadership teams evaluating technology platforms increasingly consider factors such as:
- Cloud-native architecture and operational reliability
- System availability design, including redundancy mechanisms
- Data protection frameworks that safeguard clinical and financial records
- Disaster recovery capabilities that support system restoration following major disruptions
- Operational scalability as patient volumes and service offerings expand
These considerations reflect a broader shift in healthcare technology strategy.
Infrastructure resilience is no longer viewed solely as an IT reliability issue; it is increasingly recognized as a component of enterprise operational risk management.
When clinical workflows depend on digital platforms, infrastructure architecture becomes part of the hospital’s operational resilience strategy.
Cloud-native platforms combined with structured disaster recovery frameworks allow healthcare organizations to distribute infrastructure risk across resilient cloud environments while strengthening system stability.
Operational Metrics Hospitals Should Track for System Resilience
As hospitals expand their reliance on digital systems, measuring system resilience becomes an important part of technology governance.
Operational metrics help leadership teams understand how effectively their technology environment supports continuity of care and operational coordination.
Several infrastructure and operational indicators are particularly relevant in digitally integrated hospital environments.
System Availability
System uptime remains a fundamental measure of infrastructure reliability. High system availability ensures that clinical teams can access patient information and documentation systems without interruption.
Recovery Time Objective (RTO)
RTO defines the maximum acceptable time required to restore system access following an outage. In healthcare environments where clinical workflows depend on real-time system access, shorter recovery windows are critical.
Recovery Point Objective (RPO)
RPO measures the amount of data that could potentially be lost during a system disruption. Effective disaster recovery strategies aim to minimize data loss across clinical documentation, medication records, diagnostic data, and financial transactions.
Infrastructure Incident Response Time
The time required to detect, diagnose, and resolve infrastructure incidents plays an important role in maintaining system stability.
Data Integrity and Reconciliation Efficiency
Following system disruptions, hospitals must ensure that clinical and operational records remain consistent across the system environment.
Efficient reconciliation processes help maintain data integrity and minimize administrative burden.
System resilience is increasingly measured not only by uptime, but by how quickly hospitals can detect, recover from, and stabilize operations after infrastructure disruptions.
Monitoring these metrics allows hospital leadership teams to assess whether their technology environment can sustain clinical and operational workflows under real-world conditions.
Request a Demonstration
Hospitals today rely on digital systems to coordinate clinical care, diagnostics, pharmacy services, and financial operations across multiple departments. Ensuring that these systems operate within resilient infrastructure environments is an important step toward sustaining operational continuity.
Medinous Hospital Management Software is designed as a cloud-native healthcare platform that supports integrated clinical and operational workflows while operating within secure cloud infrastructure environments that prioritize system stability and data protection.
If you would like to understand how a cloud-native Hospital Management System can support your hospital’s operational resilience and disaster recovery strategy, our team would be happy to walk you through the platform.
Request a demonstration to explore how Medinous can support your hospital’s digital health infrastructure.
Frequently Asked Questions
How does Medinous Hospital Management Software support operational continuity in hospitals?
Medinous coordinates clinical, diagnostic, pharmacy, and financial workflows within a single integrated platform. Built on a cloud-native architecture, the system enables hospitals to maintain consistent access to patient records, clinical documentation, diagnostic results, and billing workflows across distributed infrastructure environments. This helps sustain clinical workflow continuity and coordinated care delivery across departments even when infrastructure conditions become unstable.
How does Medinous support disaster recovery for hospital systems?
Medinous incorporates structured data protection and disaster recovery mechanisms designed to safeguard clinical and operational information. These capabilities help ensure that patient records, diagnostic results, medication histories, and financial transactions remain protected and recoverable. This enables hospitals to restore system availability quickly while maintaining patient data resilience.
What should hospitals consider when evaluating Medinous Hospital Management Software?
Hospitals evaluating Medinous typically assess both workflow capabilities and infrastructure reliability. Key considerations include:
• Cloud-native system architecture
• System availability and distributed infrastructure resilience
• Data protection and disaster recovery mechanisms
• Integration with diagnostic and clinical systems
• Support for coordinated clinical and administrative workflows
These factors help determine whether the platform can sustain operations within complex healthcare environments.
Can Medinous support hospitals with multi-department and multi-specialty operations?
Yes. Medinous is designed to support multi-department and multi-specialty hospital environments. The platform integrates clinical documentation, diagnostics, pharmacy services, and revenue cycle processes within a unified system environment, enabling coordinated workflows and shared access to patient information across departments.
Why should hospitals choose a cloud-native Hospital Management System such as Medinous instead of traditional systems?
Cloud-native Hospital Management Systems are designed to operate within distributed cloud environments that provide higher levels of scalability, resilience, and operational monitoring. By leveraging cloud-native architecture, hospitals can benefit from improved system availability, infrastructure redundancy, automated scaling, and structured disaster recovery capabilities, helping strengthen digital health infrastructure and clinical workflow continuity.

